
Statistically significant decreases in walking ability because of a decrease in abductor moment arm due to horizontal shortening were observed in both groups ( P=0.02, P<0.001). The average score increased from 1.8 (range, 1-3) at prefracture to 3.1 (range, 1-5) at the final follow up in 5 patients with horizontal shortening by more than 6.5 mm, and from 1.5 (range, 1-4) to 2.3 (range, 1-5) in 20 patients with horizontal shortening less than 6.5 mm. On average, walking ability decreased 1 step ( Table 2). The average score increased from 2.0 at pre-fracture to 2.9 at the final follow up. However, at the final follow up, these changed to 5, 15 and 5 cases, respectively. Using the Koval classification 20), walking ability of the patients before surgeries were as follows independent community ambulatory (grade 1 n=12), community ambulatory with cane (grade 2 n=10), household ambulatory independently or with assistive devices (n=3). Pre-fracture and final follow-up ambulatory levels were evaluated as a clinical parameter according to the Koval classiflcation 20) which grades ambulatory ability from independent community ambulatory (grade 1) to nonfunctional ambulatory (grade 7). We also examined patients to determine if other complications were present. To assess decreases in abductor moment arm, the difference in length between the healthy and unhealthy sides (horizontal shortening) was quantified by measuring the distance from medial border of the femoral head to lateral border of the greater trochanter at the final follow-up radiography visit following bone union 17) ( Fig. Nonunion was defined as: i) displacement of the fracture site by more than 1 cm without fracture union, ii) change in the angle of cannulated screws by more than 5%, iii) screw or blade back-out by more than 2 cm, or iv) femoral perforation these measurements were made at the 3-month follow-up radiography visits 19). Using radiography, union at the fracture site was checked at follow-up on a regular basis. Stable femoral neck fractures were defined as Garden types 1 and 2 according to the Garden classification 18) 16 were type 1 and 9 were type 2. The average follow-up period was 32 months (range, 12-183 months). Bone mineral density test was performed in 20 cases 16 had osteoporosis and 4 had osteopenia. The average body mass index was 22.1 kg/m 2 (range, 16.0-29.6 kg/m 2). Five of the subjects were men and the remaining 20 were women their mean age was 72.3 years (range, 65-84 years) at the time of surgery. Fractures occurred after a slip or fall accident in all but 1 case. The remaining 25 patients with a minimum follow-up of 1 year were included in this retrospective study. 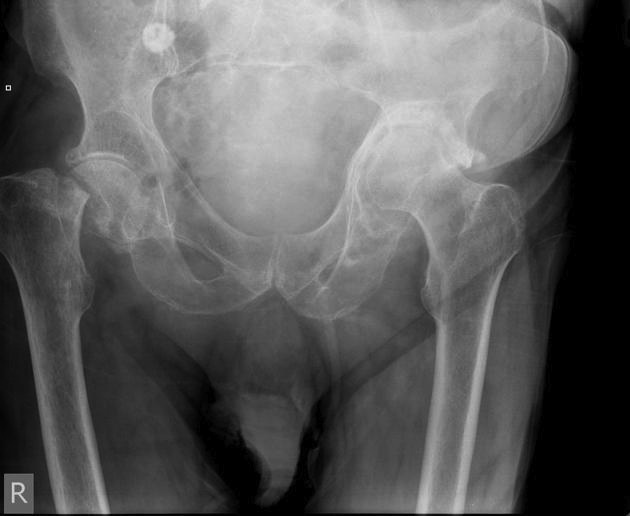
Of these, 6 were excluded because of death within 1 year due to underlying disease regardless of fracture surgery (n=3) or because they were not available for follow ups (n=3). Thirty-one patients were age 65 years or older and considered for this study. Eighty-five patients underwent internal fixation for femoral neck fracture from January 2008 to December 2014. We obtained the approval from institutional review board of Keimyung University Dongsan Medical Center to search surgical database of our institution to identify cases for the current study. For these reasons, the optimal treatment strategy for elderly patients with stable femoral neck fractures remains unclear. Others have suggested that a postoperative decrease in abductor moment arm may reduce mobility and quality of life 17). However, some authors have reported a high re-operation rate in older patients with undisplaced fractures, because of fixation failure, avascular necrosis of the femoral head and others 13 14 15 16). Additionally, internal fixation has traditionally been the preferred method for treating incomplete fractures, stable fractures (Garden type 1) or undisplaced fractures (Garden type 2) regardless of age, and satisfactory outcomes have been achieved including relatively short operation time and joint preservation 9 10 11 12). Internal fixation is considered a better treatment choice for younger patients 7 8). Compared to internal fixation, hip arthroplasty is more commonly performed in elderly patients with displaced femoral neck fractures because of more significant improvements in pain and early ambulation, lower rates of re-operation and other advantages 4 5 6). Fracture site displacement, patient age, comorbid disorders, pre-fracture activity level are some of the critical factors in determining the clinical practice for treating femoral neck fractures 3). The incidence of femoral neck fractures, one of the leading causes of death in elderly patients is increasing as average life spans and prevalence of osteoporosis continue to rise 1 2).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
